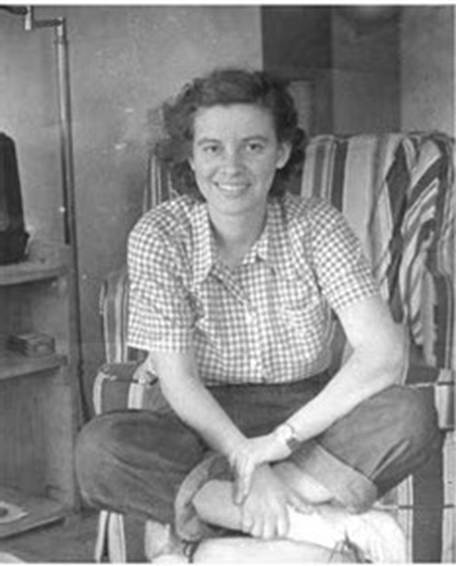In 1967, Pittsburgh’s Hill District was a community abandoned by the systems meant to protect it. When residents suffered heart attacks, accidents, or medical emergencies, they often waited in vain for help that never arrived with adequate care. The predominantly Black and impoverished neighborhood had been systematically ignored by city services, including emergency medical transport. But from this injustice emerged a revolution that would transform emergency medicine across America—only to be deliberately erased from history.
Freedom House Ambulance Service began as a bold experiment in community empowerment and medical innovation. Founded by the Maurice Falk Fund president Phil Hallen and Dr. Peter Safar—whose own daughter had died after an asthma attack during inadequate emergency transport—the service recruited twenty-five Black men from the Hill District. Most were unemployed, some were Vietnam veterans struggling with addiction, and many had been labeled “unemployable” by city welfare offices. They were the kind of men society had written off.
What happened next was extraordinary. Under Dr. Safar’s guidance, these recruits underwent an intensive 32-week, 300-hour training program covering anatomy, physiology, CPR, advanced first aid, nursing, and defensive driving. This wasn’t basic first aid—it was medical training at a level that simply didn’t exist anywhere in the United States at that time. When Freedom House officially began operations in 1968, these men became America’s first true paramedics.
The impact was immediate and profound. In their first year alone, Freedom House responded to nearly 6,000 calls, transported more than 4,600 patients, and saved an estimated 200 lives. Their response time was under ten minutes in most neighborhoods, a stark contrast to the slow or non-existent service residents had endured before. The paramedics became the first to perform intubation in the field, to use defibrillators outside hospitals, and to transmit medical data via radio while transporting patients. They transformed ambulances from mere transport vehicles into mobile treatment centers.
Dr. Nancy Caroline joined as medical director in 1974, further expanding the training curriculum and writing what would become the first paramedic textbook, still used as the basis for emergency medical training today. The National Highway Traffic Safety Administration adopted Freedom House’s ambulance model as the official standard for the United States in 1975. The service had become a national model, proof that with proper training and support, communities could transform their own futures.

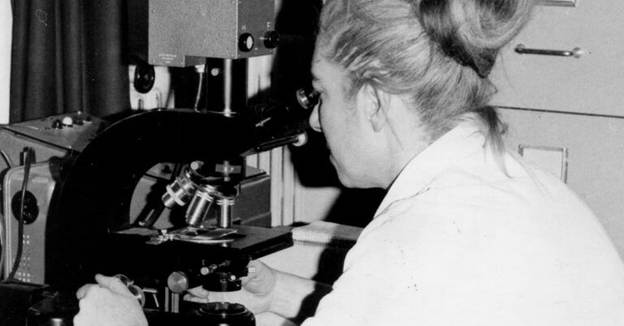
Dr, Nancy Caroline, Medical Director, Freedom House Ambulance Service
But success couldn’t shield Freedom House from the racism embedded in Pittsburgh’s power structure. As white neighborhoods learned that the Hill District was receiving superior emergency care, resentment grew. Rather than expanding Freedom House’s services citywide, Mayor Peter Flaherty made a different choice. In 1975, he announced the creation of a city-run ambulance service and cut Freedom House’s funding, forcing it to cease operations after just eight years.
What followed was a systematic erasure. Though city officials promised to hire the Freedom House paramedics, the reality was crueler. Many were forced to take pass/fail exams covering material they’d never been taught. Of the 26 Freedom House employees who joined the city service, only half remained after a year. Most were reassigned to non-medical duties or placed under white supervisors with less experience. Ultimately, only five stayed long-term, and just one reached a leadership position. By the late 1990s, 98 percent of Pittsburgh’s Bureau of Emergency Medical Services was white.
The history books largely forgot them. Textbooks taught the methods they pioneered without mentioning their names. Paramedics across the nation used the curriculum they developed, unaware of its origins in a predominantly Black neighborhood fighting for dignity and survival.
Freedom House Ambulance Service represents both the heights of innovation and the depths of institutional racism. These paramedics saved lives, revolutionized emergency medicine, and proved what marginalized communities could achieve when given resources and respect. In return, they were fired, replaced, and deliberately written out of the history they created.
Their story is a reminder that progress in America has often been built on Black innovation, and that those contributions have too often been appropriated, credited to others, or simply forgotten. Recognizing Freedom House today isn’t just about honoring the past. It’s about acknowledging whose knowledge we’ve stolen, whose labor we’ve exploited, and whose stories we’re still failing to tell.