Purdue Pharma, The Sackler Family, and the Opioid Crisis
How a pharmaceutical empire was built — and what it cost millions of Americans
A Note to Our Readers: This article is written with deep respect for the millions of people living with chronic pain and for those whose lives have been touched by addiction. Pain is real. Suffering is real. The story told here is not a condemnation of patients — it is an examination of corporate and regulatory failures that harmed both those who needed relief and those who were led into dependency. If you or someone you love is navigating pain management or recovery, please know you are seen, and your experience matters.
Introduction: A Crisis That Didn’t Have to Happen
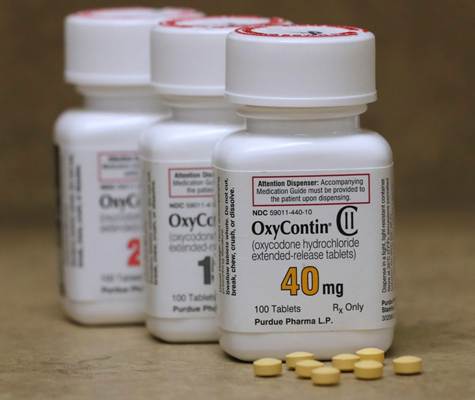
Few chapters in American medical history are as tragic or as preventable as the opioid epidemic. At its center is a single drug: OxyContin. Around that drug, a story of extraordinary ambition, willful blindness, corporate deception, regulatory failure, and, ultimately, devastating human cost.
For the people most deeply affected, chronic pain patients who relied on opioids to live functional lives, individuals who became dependent or addicted through no fault of their own, and the families torn apart by overdose, the OxyContin saga is not an abstraction. It is personal. It is lived. And for many, it continues today in the form of restricted access to medications that genuinely help, stigmatized clinical relationships, and a pain management landscape that remains fractured by the consequences of Purdue Pharma’s choices.
This is the story of how OxyContin was developed, how it was marketed through one of the most aggressive and deceptive pharmaceutical campaigns in history, how addiction and overdose deaths followed, and how the Sackler family, the billionaires who owned Purdue Pharma , used the legal system to shield their fortune while the communities they helped devastate were left to rebuild on their own.
Part One: The Origins of OxyContin
Purdue Pharma and the Sackler Dynasty

Purdue Pharma was founded in 1892 as a small New York medical publisher, but its transformation into a pharmaceutical powerhouse began when the Sackler family entered the picture. Arthur, Mortimer, and Raymond Sackler were three brothers who became wealthy through advertising, psychiatry, and pharmaceutical marketing in the mid-20th century. Arthur Sackler, in particular, was a pioneering force in direct-to-physician drug marketing, a model that would later prove catastrophic in Purdue’s hands.
After Arthur Sackler’s death in 1987, his portion of the company was sold to his brothers, leaving Mortimer and Raymond — and eventually their descendants — in full control of Purdue Pharma. The family operated the company privately, shielding its finances from public scrutiny for decades.
MS Contin and the Road to OxyContin
Before OxyContin, Purdue had found success with MS Contin, a controlled-release morphine tablet for cancer pain. MS Contin was genuinely useful for patients in severe, end-of-life pain, and it gave Purdue Pharma both a revenue stream and a template — the idea that extended-release opioids were a viable and even superior product to short-acting formulations.
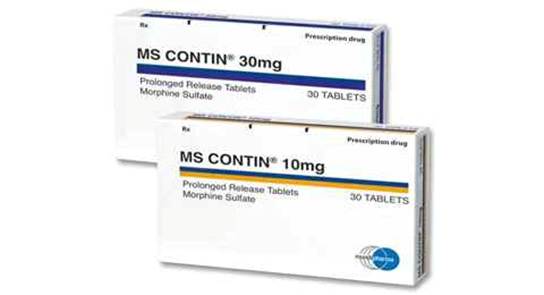
When the MS Contin patent was approaching expiration in the mid-1990s, Purdue needed a new product. The result was OxyContin: oxycodone in a patented extended-release formulation, marketed as providing 12 hours of continuous pain relief from a single tablet. The drug was approved by the FDA in December 1995 and launched in 1996.
The Science Behind the Drug
Oxycodone itself was not new. It had been used in combination products like Percocet for decades. What Purdue claimed was new was the delivery mechanism: a wax matrix coating that, in theory, released the drug slowly over 12 hours. The FDA, in approving OxyContin, accepted Purdue’s claim that the extended-release formulation made the drug less prone to abuse than immediate-release opioids, an assertion that would later be exposed as unfounded and, arguably, deliberately misleading.
Critically, many patients found that the drug’s effects wore off well before 12 hours, leading physicians to prescribe more frequent dosing and inadvertently increasing exposure. And for those who learned to crush the tablet, the extended-release coating became irrelevant, releasing a powerful dose of oxycodone all at once.
Part Two: The Marketing Campaign — A Masterwork of Deception
The ‘1% Addiction’ Myth
Perhaps no single piece of misinformation did more damage than the claim Purdue’s sales force repeatedly made to physicians: that fewer than 1% of patients prescribed OxyContin for pain would develop addiction. This figure originated from a brief letter published in the New England Journal of Medicine in 1980, which reported that addiction was rare among hospitalized patients given narcotic medications. It was not a clinical study. It did not examine long-term outpatient use. It did not define addiction rigorously. Yet Purdue’s representatives cited it thousands of times as scientific proof that OxyContin was “not addictive” when used for pain.
“We have to hammer on the abusers in every way possible. They are the culprits and the problem. They exist in every community and must be identified to your doctors so they can be treated for their obvious problem.” — Internal Purdue Pharma communication to sales staff, circa 2001
This narrative was central to Purdue’s commercial strategy. By reassuring physicians that addiction risk was negligible, the company could encourage broader prescribing not just for cancer pain, the traditional domain of strong opioids, but for common chronic conditions like back pain, arthritis, and fibromyalgia. The market expansion was deliberate and dramatic.
Targeting Physicians and Building a Sales Force
Purdue deployed one of the largest and most aggressive pharmaceutical sales forces the industry had seen for a single drug. By the late 1990s, hundreds of sales representatives were visiting physician offices across the country, with particular focus on high-prescribing pain specialists, general practitioners in rural and post-industrial communities, and physicians who were unfamiliar with the risks of opioid therapy.
Sales representatives were incentivized through a bonus structure tied directly to the number of OxyContin prescriptions written in their territories. The more prescriptions, the larger the bonus. Some representatives earned tens of thousands of dollars annually in bonuses alone. Internal documents later revealed that Purdue was fully aware which physicians were prescribing at unusually high volumes, so-called “pill mills”, and in many cases, continued to send representatives to those offices rather than reporting concerns.
Gifts, Meals, and Sponsored Education
The campaign extended far beyond sales calls. Purdue sponsored thousands of pain management seminars at resorts and vacation destinations, flew physicians to training conferences, and distributed branded merchandise. Doctors received gifts, meals, and speaking fees. The company created patient education materials emphasizing the benefits of treating pain aggressively and distributed literature that reinforced the message that undertreated pain was a crisis, and opioids were the solution.
Purdue also cultivated relationships with pain advocacy organizations, some of which received funding from the company, and whose public messaging often aligned closely with Purdue’s commercial interests. The medical and regulatory establishment was, in many ways, swimming in the same waters, creating an environment in which critical scrutiny of OxyContin’s risks was slower to emerge than it should have been.
The ‘Pseudoaddiction’ Concept
When patients began showing signs of physical dependence and asking for higher doses, becoming distressed when prescriptions were delayed, or visiting multiple physicians, some Purdue-affiliated clinicians promoted a concept called “pseudoaddiction.” The idea was that these behaviors were not signs of addiction, but signs of undertreated pain. The solution, in this framework, was not to taper or reconsider the patient’s opioid use, but to prescribe more.
This concept, whatever its original intent in the medical literature, was weaponized commercially to deflect concerns about dependency and to encourage continued high-dose prescribing. It also placed the burden of suspicion on the patient, suggesting that concern about a patient’s opioid use was itself a form of undertreatment.
Part Three: The Human Cost — Addiction, Overdose, and the Collapse of Trust
The Epidemic Takes Hold
The consequences of Purdue’s campaign unfolded gradually and then catastrophically. OxyContin sales reached approximately $45 million in 1996, Purdue’s first year. By 2000, annual sales exceeded $1 billion. By the mid-2000s, OxyContin was generating more than $3 billion a year, and it had become the best-selling opioid painkiller in the United States.
During the same period, opioid overdose deaths began rising steeply. Emergency rooms in states like West Virginia, Kentucky, Ohio, and Virginia, areas with high concentrations of industrial workers and limited healthcare infrastructure, began reporting alarming numbers of patients in respiratory crisis. Pharmacies reported shortages. Addiction treatment centers were overwhelmed. Families buried parents, children, and siblings.
The Collateral Damage to Legitimate Pain Patients
What is often missing from the public narrative and what is deeply important for the chronic pain community is this: not everyone who took OxyContin became addicted. Many patients used it responsibly, under physician supervision, and it meaningfully reduced their suffering. Opioid medications, when carefully prescribed and monitored, remain essential tools for treating serious chronic pain.
But as the epidemic grew and regulatory and law enforcement scrutiny intensified, the pendulum began to swing sharply in the other direction. Physicians, fearing DEA investigations and license revocations, began tapering or abruptly stopping opioid prescriptions. Pharmacies became reluctant to fill opioid prescriptions. New guidelines including the controversial 2016 CDC opioid prescribing guidelines, which were subsequently widely misapplied, created an environment in which legitimate pain patients found themselves abruptly cut off from medications they had depended on for years.
The tragedy of the opioid crisis is that it harmed people at both ends: those who became addicted to medications they were told were safe, and those with genuine pain who were later denied treatment because of the failures of the system that harmed the former.
Patients with cancer pain, neuropathic pain, spinal conditions, and other serious diagnoses described being made to feel like criminals for requesting medication. Doctor-patient relationships built over years were severed. Some patients, denied their medications, turned to illicit opioids — often laced with fentanyl — and died. The collateral damage of the crisis, in other words, ran in more than one direction.
The Role of Diverted Medications and Pill Mills
It would be incomplete to tell this story without acknowledging that diversion, the sale and distribution of legitimately prescribed opioids outside the medical system, was a major driver of the epidemic. Some physicians, whether motivated by greed or negligence, operated practices that functioned as pill mills, prescribing opioids to virtually anyone who walked in the door. Purdue Pharma, as noted, often knew who these physicians were. DEA and state regulators, meanwhile, were slow to act.
The result was that OxyContin and other opioids flooded communities, schools, and social networks. For many people who became addicted, the first exposure was not a physician’s prescription but a pill from a friend, a family member, or a dealer. The drug did not respect the boundaries of the original patient population.
Part Four: The Reckoning — Legal Action Against Purdue and the Sacklers
Early Legal Troubles (2007)
Purdue Pharma was not unaware of the storm gathering around it. Internal documents from the late 1990s and early 2000s, later revealed in litigation and investigative journalism, show that company executives were informed of reports of addiction, overdose, and diversion, and in many cases chose to manage those reports through public relations rather than reforming their marketing practices.
In 2007, Purdue Pharma and three of its top executives, including President Michael Friedman, Chief Legal Officer Howard Udell, and former Chief Medical Officer Paul Goldenheim, pleaded guilty to federal criminal charges of misbranding, having misled the public about OxyContin’s abuse potential. The company was fined $600 million, and the executives paid approximately $34 million in fines. It was, at the time, one of the largest criminal fines ever levied against a pharmaceutical company.

From left, Howard R. Udell, the top lawyer for Purdue Pharma; Dr. Paul D. Goldenheim, the company’s former medical director; and Michael Friedman, Purdue’s president.
But the 2007 settlement was, in retrospect, a settlement that allowed Purdue and the Sacklers to continue operating. No executives went to prison. The company continued selling OxyContin. Sales continued to grow.
The Wave of State and Federal Lawsuits
Beginning around 2017, a wave of lawsuits from states, counties, cities, Native American tribes, and other entities began to converge on Purdue Pharma and the Sackler family personally. Attorneys general from nearly every state sued, as did thousands of local governments. The litigation drew on a model pioneered in tobacco litigation: holding a corporation responsible not just for a defective product but for a deliberate, knowing marketing strategy that caused widespread public harm.
Internal documents obtained in discovery, many of which were initially sealed but eventually made public, in part due to the efforts of investigative journalists and state attorneys general , revealed the extent of Purdue’s knowledge of OxyContin’s harms and the aggressiveness with which it had suppressed and managed those concerns. Email chains among Sackler family members showed direct involvement in sales strategy and a persistent focus on revenue growth even as overdose deaths mounted.

The Sackler Family’s Financial Maneuvering
What became clear through litigation was that members of the Sackler family had, over the preceding decade, extracted enormous sums of money from Purdue Pharma. Between roughly 2008 and 2018, the Sackler family received an estimated $10 to $13 billion in distributions from the company. Much of this money was transferred to entities and accounts outside the United States — in Switzerland, in offshore trusts, and in other structures that complicated any effort to claw it back through bankruptcy proceedings.
This financial maneuvering — which plaintiffs’ attorneys characterized as a deliberate strategy to protect family assets from litigation — became one of the central controversies of the bankruptcy proceedings that followed.
Purdue’s Bankruptcy and the Controversial Settlement
In September 2019, facing an overwhelming tide of litigation, Purdue Pharma filed for Chapter 11 bankruptcy. The filing triggered a complex legal process in which the company sought to resolve all claims against it through a single settlement rather than face individual lawsuits in courts around the country.
The settlement that emerged from the bankruptcy process offered states and plaintiffs billions of dollars — ultimately on the order of $6 billion from Sackler family members, along with the dissolution of Purdue Pharma and the creation of a new entity, Knoa Pharma, which would make its profits available for opioid abatement. The settlement also included a sweeping provision that granted members of the Sackler family broad legal immunity from future civil suits related to OxyContin — a provision that did not require the Sacklers to file for personal bankruptcy or admit any wrongdoing.
This immunity provision became extraordinarily controversial. Critics including several state attorneys general, legal scholars, and eventually the U.S. Trustee’s office argued that extending bankruptcy protection to individuals who had not themselves filed for bankruptcy was an abuse of the bankruptcy process and fundamentally unfair to victims who would lose their right to pursue the Sacklers individually in court.
The settlement allowed some of the wealthiest people in America to buy legal immunity without ever being held personally accountable in a court of law.
The Supreme Court Weighs In
The legal battle over the Sackler immunity provision reached the United States Supreme Court. In June 2024, in a 5-4 decision in Harrington v. Purdue Pharma L.P., the Supreme Court ruled that the bankruptcy settlement’s provision shielding the Sackler family from civil liability was impermissible. The majority held that bankruptcy courts do not have the authority to grant such broad immunity to third parties who have not themselves filed for bankruptcy and who have not made all of their assets available to creditors.
The ruling sent the case back to lower courts for renegotiation. It was a significant legal victory for victims and for the principle that wealth cannot simply purchase immunity. However, the practical consequences of the ruling remain uncertain: new negotiations between the Sacklers, states, and victim groups have continued, and any revised settlement must still thread the needle between compensation for victims and the legal and financial realities of what remains recoverable.
Criminal Accountability — and Its Limits
In addition to civil litigation, federal criminal investigations yielded a guilty plea from Purdue Pharma as a corporation in 2020, with the company admitting to felony charges related to its marketing practices. The plea agreement included an $8.3 billion resolution — the largest settlement of its kind in U.S. history though much of this sum was contingent on the outcome of the bankruptcy proceedings and may never be fully collected.
What has been notably absent from the accountability process is criminal prosecution of individual Sackler family members. Despite the extraordinary evidence of their personal involvement in Purdue’s marketing strategy and their knowledge of its consequences, no family member has faced criminal charges. This stands in stark contrast to the treatment of lower-level participants in the opioid supply chain — physicians, pharmacists, and street-level distributors — who have faced federal prosecution and prison sentences.
Part Five: Where Things Stand Today
The Sackler Family’s Wealth and Reputation
Despite the legal proceedings, members of the Sackler family remain wealthy. Their personal fortunes, estimated at several billion dollars even after settlement payments, are intact. Many family members have stepped back from public view, and several major cultural institutions, the Louvre, the Smithsonian, the Guggenheim, Harvard, Oxford, the Tate, have removed the Sackler name from buildings and galleries in response to public pressure. These symbolic gestures represent a form of accountability, but a limited one.

The State of Pain Management
For chronic pain patients and their physicians, the aftermath of the opioid crisis has created a landscape that is, in many ways, more difficult than before. The 2016 CDC guidelines, though intended to reduce overprescribing, were widely misinterpreted as prescribing limits rather than voluntary guidelines, leading to abrupt tapering, prescription abandonment, and genuine suffering among patients who had no alternative.
In 2022, the CDC revised its guidelines and explicitly acknowledged that they had been misapplied; that the intent was never to create mandatory dose limits, and that patients with legitimate chronic pain conditions should not be abruptly denied effective treatment. But the culture of fear that had developed among prescribers, fear of DEA investigation, fear of liability, has not disappeared overnight.
Many pain specialists report that their practices are now shaped as much by regulatory anxiety as by patient need. Patients with cancer, autoimmune conditions, spinal injuries, and other serious diagnoses continue to describe difficulty accessing opioid medications, long waits for pain specialists, and a clinical environment in which their descriptions of pain are met with suspicion rather than compassion.
The Ongoing Opioid Crisis
The opioid epidemic itself has not ended. In fact, in the years since OxyContin became notorious, the nature of the crisis shifted dramatically. As prescription opioids became harder to obtain — through prescription drug monitoring programs, pill mill crackdowns, and reformulated abuse-deterrent versions of OxyContin — many people with opioid use disorder transitioned to heroin. And then, as illicit fentanyl flooded the drug supply, overdose deaths accelerated rather than declined.
More than 80,000 Americans died from opioid overdoses in 2023, the vast majority involving illicit fentanyl. The story that began with a deceptive pharmaceutical marketing campaign is now, in many ways, a public health crisis of a different character — one driven by a contaminated illicit drug supply, inadequate access to addiction treatment, and the social and economic conditions that make people vulnerable to substance use disorder.
Victims and the Compensation Process
The abatement funds created through the Purdue bankruptcy proceedings and other opioid-related settlements, including large settlements with distributors McKesson, Cardinal Health, and AmerisourceBergen, and manufacturer Johnson & Johnson, have made billions of dollars available to states and localities for opioid treatment and prevention programs. Whether those funds are being deployed effectively, and whether they reach the most deeply affected communities, remains an active question.
Individual victims and families who lost loved ones to opioid overdose have received comparatively small amounts from settlement funds, and many have expressed frustration that the compensation process has been slow, complex, and insufficiently transparent. The human cost of the epidemic — measured in lives lost, families fractured, communities hollowed out — is not reducible to any dollar figure.
Conclusion: Lessons, Accountability, and the Path Forward
The OxyContin saga is, at its core, a story about what happens when the profit motive overwhelms both medical ethics and regulatory oversight. Purdue Pharma did not create the concept of pharmaceutical corruption, and it will not be the last company to put earnings above patient safety. But the scale of harm it helped engineer, the sophistication of its deception, and the extraordinary wealth it accumulated while that harm unfolded make it one of the defining corporate scandals of our era.
For chronic pain patients, the legacy is bitter in a particular way. Pain patients were not the architects of this crisis. Many were simply people trying to manage debilitating conditions with the medications their doctors prescribed. They were caught between Purdue’s deception and the regulatory backlash it eventually triggered — used as a market, then abandoned when the market became a liability.
For physicians trying to provide compassionate, evidence-based care to patients in pain, the legacy is a clinical environment warped by liability concerns and public stigma. Good pain management has become harder to practice in the long shadow of Purdue’s choices.
The path forward requires holding both truths simultaneously: that opioids were recklessly overprescribed in ways that caused immense harm, and that opioids remain essential medications for many patients with serious pain conditions. That addiction is a medical condition deserving of treatment, not punishment. And that corporate accountability — including personal accountability for the individuals who made the decisions — is not optional in a functional society.
The Supreme Court’s ruling blocking the Sackler immunity provision was a step toward that accountability. It was not the last word. The renegotiation of the settlement, the deployment of abatement funds, and the long work of rebuilding trust in pain medicine will all continue for years to come.
The patients who suffered deserve better than what they got. So do the communities that are still rebuilding. And the least that accountability requires is that the people responsible face genuine consequences — not just a negotiated exit.
Resources
If you are a chronic pain patient struggling to access appropriate care, organizations such as the American Chronic Pain Association (theacpa.org) and the American Pain Society can provide guidance and advocacy resources.
If you or someone you love is struggling with opioid use disorder, SAMHSA’s National Helpline (1-800-662-4357) provides free, confidential, 24/7 treatment referral and information.
For those seeking to understand the legal proceedings in depth, the reporting of Beth Macy (Dopesick), Patrick Radden Keefe (Empire of Pain), and the investigative teams at ProPublica and The New York Times have produced essential journalism on this subject.
— End —
Leave a comment